Neurochemical Patterns in TAS
- Mint Achanaiyakul
- 30 minutes ago
- 7 min read
How dopamine, serotonin, and norepinephrine shape the Trauma-Adaptive Spectrum Model
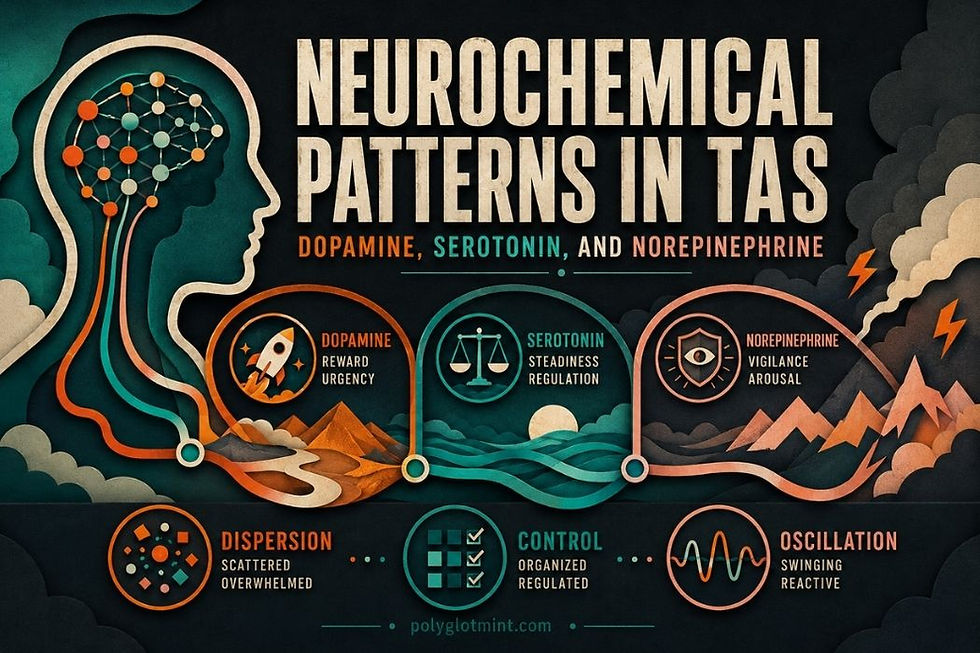
© Mint Achanaiyakul — Founder of Crimson Cat Events & Psychomedia
The Trauma-Adaptive Spectrum Model argues that ADHD-, OCD-, and bipolar-like patterns may be better understood as neighboring adaptive states within one broader dysregulated system. This companion article focuses on the neurochemical side of that claim.
It does not argue that each diagnosis maps neatly onto one neurotransmitter. The brain is not that tidy. Instead, it proposes that unstable patterns across reward, regulation, and vigilance systems may help explain why one person leans toward attentional dispersion, another toward compulsive control, and another toward oscillation between activation and collapse.
Neurochemical patterns in TAS begin with instability
The core point is not that people have “good chemicals” or “bad chemicals.” The point is instability.
According to van der Kolk (2003) in The Neurobiology of Childhood Trauma and Abuse, trauma changes what children anticipate, focus on, and how they organize appraisal and regulation. According to Teicher and Samson (2016) in Annual Research Review: Enduring Neurobiological Effects of Childhood Abuse and Neglect, childhood maltreatment has lasting effects on brain development and many changes later associated with psychiatric illness may be direct consequences of abuse and neglect. Within TAS, neurochemical dysregulation is therefore not treated as floating free of life experience. It is treated as part of what chronic instability, unsafe communication, and repeated threat do to a nervous system over time.
Dopamine and the search for regulation
Dopamine is the clearest starting point because it helps explain why dysregulated states can become so compelling. According to Schultz (2016) in Dopamine Reward Prediction Error Coding, dopamine is deeply involved in reward prediction, learning, and updating behavior when something important or unexpected happens. Within TAS, that matters because a nervous system shaped by instability may stop responding to ordinary life with steady motivation and instead become biased toward urgency, certainty, intensity, or whatever brings temporary regulation fastest.
This is what reward dysregulation means in practical terms. Ordinary life no longer produces stable enough motivation, satisfaction, or calm. Routine tasks lose pull. Low-stimulation activities feel hard to enter or sustain. Relief, novelty, certainty, or emotional intensity begin to feel disproportionately regulating, so the nervous system starts repeating whatever restores control or aliveness most quickly.
In ADHD-like patterns, this may look like drifting through repetitive work, avoiding low-stimulation tasks, switching tabs, chasing urgency, or only being able to focus once a deadline becomes immediate. In OCD-like patterns, it may look like checking, rereading, arranging, replaying, or ritualizing because repetition briefly restores certainty. In bipolar-like patterns, unstable reward signaling may help intensify periods of amplified drive, reduced need for rest, overcommitment, and momentum, followed by collapse, depletion, or dysphoria.
This reward-seeking logic also aligns with The Dopamine Paradigm†, which further develops how unstable reward signaling can drive compensatory, self-reinforcing behavior.
Serotonin and the stability problem
If dopamine helps explain drive, salience, and urgency, serotonin helps explain steadiness.
Within TAS, reduced serotonergic stability helps explain why uncertainty can become harder to tolerate, why emotional regulation weakens, and why inhibition may fail under stress. The point is not that serotonin alone “causes” OCD, depression, or bipolar disorder. The point is that when serotonergic stability is compromised, the nervous system may have less capacity to stay emotionally even, delay reaction, tolerate ambiguity, or remain settled under internal pressure.
That matters because TAS is not only a theory of activation. It is also a theory of failed steadiness. A dysregulated system does not simply seek more stimulation. It often also loses the ability to remain regulated in the absence of stimulation. That is one reason repetition, urgency, and certainty can begin to feel so necessary.
Norepinephrine and chronic vigilance
The third major player in this companion model is norepinephrine. If dopamine helps explain reward and serotonin helps explain steadiness, norepinephrine helps explain vigilance.
Norepinephrine is central to alertness, arousal, and readiness under stress. Within TAS, stress-linked noradrenergic activation helps explain why people become distractible under pressure, hyper-attentive to threat, easily overstimulated, or unable to settle their attention once the nervous system has learned that the environment is unreliable.
This matters especially for trauma-shaped ADHD-like dispersion. A scattered mind is not always under-motivated. Sometimes it is over-alert. It keeps scanning because scanning once helped it survive. In this sense, attentional problems may reflect not only “low focus,” but a nervous system that has learned to remain partially mobilized.
Neurochemical patterns in TAS are not one-to-one diagnoses
The model gets weaker, not stronger, if it pretends to be a clean conversion chart. It is not:
dopamine = ADHD
serotonin = OCD
norepinephrine = bipolar
That would be too crude.
According to Salvi et al. (2021) in ADHD and Bipolar Disorder in Adulthood: Clinical and Treatment Implications, ADHD and bipolar disorder overlap substantially and are clinically difficult to separate cleanly in some cases. That matters because TAS is not arguing for isolated chemical diseases. It is arguing that one dysregulated system can express itself through different dominant adaptive patterns depending on which regulatory strategies become most reinforced.
Within TAS, these adaptive patterns may coexist in the same person at different intensities, and two or more may be strongly present at the same time even when one is more dominant overall. Neurochemical instability helps explain why that blending happens.
Table 1. Neurochemical Patterns in TAS
Neurochemical pattern | Regulatory effect | Common adaptive behavior | Possible TAS expression |
Low or unstable dopamine signaling | Weak steady motivation, urgency dependence, novelty-seeking | scanning, stimulation-seeking, impulsive switching | ADHD-like dispersion |
Dopamine relief through repetition plus low tolerance for uncertainty | Temporary certainty restoration through repeated action | checking, arranging, rereading, replaying | OCD-like compulsion |
Unstable reward activation followed by depletion | amplified drive, then collapse | overcommitment, reduced rest, later crash | bipolar-like oscillation |
Stress-linked noradrenergic activation | vigilance, distractibility, threat scanning | overstimulation, reactivity, inability to settle | cross-pattern intensification |
Reduced serotonergic stability | weakened inhibition, lower emotional steadiness | intolerance of ambiguity, reactivity, regulation difficulty | cross-pattern intensification |
This table is not meant to assign people to neat biochemical boxes. It is meant to show how different forms of instability can reinforce different adaptive behaviors within one broader spectrum.
Reinforcement is where chemistry becomes behavior
Neurochemical instability matters because it changes what feels relieving enough to repeat.
If a behavior briefly reduces overwhelm, it is more likely to be reused. If it briefly restores certainty, it is more likely to be reused. If it brings stimulation to a depleted system, it is more likely to be reused. That is the bridge between chemistry and habit, and between habit and symptom pattern.
This is also why TAS does not treat mental illness as random defect. According to Teicher et al. (2010) in Hurtful Words: Association of Exposure to Peer Verbal Abuse With Elevated Psychiatric Symptom Scores and Corpus Callosum Abnormalities, harmful language is associated with elevated psychiatric symptoms and structural differences in language-related pathways. Within TAS, repeated criticism, contempt, contradiction, and coercive tone are not just emotionally painful. They are part of the regulatory environment shaping what the nervous system learns to repeat.
Media as original training ground, not just amplifier
One of the most important implications of Psychomedia is that media does not only intensify preexisting dysregulation. It can also function as an original training ground.
According to Lang (2000) in The Limited Capacity Model of Motivated Mediated Message Processing, the structure of mediated messages shapes attention and memory allocation. According to Meshi et al. (2013) in Nucleus Accumbens Response to Gains in Reputation for the Self Relative to Gains for Others Predicts Social Media Use, reward-related brain activity is implicated in social-media use. TAS extends this by arguing that social media, films, television, advertising, and songs can train urgency, repetition, comparison, emotional volatility, and unstable reward patterns from the start.
Media is therefore not just content. It is reinforcement architecture. It repeatedly pairs attention with threat, reward with humiliation, stimulation with dependency, and desire with instability. In that sense, media can help install the very patterns it later appears merely to reflect.
This is also why media can program the Language of Abuse† into us. Repeated exposure to contradiction, degradation, volatility, and unstable reward can train the same emotional grammar that traumatized environments teach in interpersonal life.
Neurochemical patterns in TAS and the Sex–Death pull
Within the broader framework of Duality of Neural Programming (DNP), these neurochemical patterns often bias the nervous system toward the Sex–Death Circuit: urgency, compulsion, stimulation, comparison, instability, and survival-coded intensity.
From this perspective, dysregulation is not only a clinical issue. It is directional. The system is repeatedly trained toward whatever is fastest, loudest, most urgent, or most chemically relieving, even when that movement deepens instability.
Recovery means retraining the pattern
If breakdown is reinforced, recovery must also be reinforced.
That means the neurochemical story cannot stop at dysregulation. It must also ask how steadier regulation gets rebuilt. Within TAS, recovery is not just the suppression of symptoms. It is the retraining of reward, expectation, language, rhythm, and safety.
Predictable connection matters. Safer language matters. Lower-stimulation environments matter. Bonding matters. Coherent reward matters. What is being rebuilt is not only behavior, but the nervous system’s expectation of what life feels like when it is no longer organized around urgency, compulsion, collapse, and threat.
Why this companion article matters
The point of this article is not to reduce people to chemicals. It is to clarify how chemistry, trauma, reinforcement, and environment fit together inside TAS.
Mental illness does not need to be imagined as a collection of sealed disorders with sealed mechanisms. It may make more sense as a broader dysregulated system expressing itself through different adaptive strategies depending on what has been reinforced, what has been deprived, and what the nervous system has learned to expect.
That is the neurochemical logic of TAS.
Read the full pillar article here:
Notes on Novelty
This companion article clarifies the neurochemical logic underlying the Trauma-Adaptive Spectrum Model. Rather than mapping diagnoses onto isolated chemicals, it frames dopamine, serotonin, and norepinephrine as interacting regulatory systems whose instability may reinforce different dominant adaptive patterns.
It also extends Psychomedia’s argument by treating media not only as an amplifier of dysregulation, but as an original conditioning environment capable of training urgency, repetition, comparison, and unstable reward patterns from the start.
† Indicates a forthcoming work or internal cross-reference within the Psychomedia framework.
Achanaiyakul, M. (2026). Neurochemical Patterns in TAS. PolyglotMint.com.
References
van der Kolk, 2003. The Neurobiology of Childhood Trauma and Abuse. (Child and Adolescent Psychiatric Clinics of North America)
Teicher and Samson, 2016. Annual Research Review: Enduring Neurobiological Effects of Childhood Abuse and Neglect. (Journal of Child Psychology and Psychiatry)
Schultz, 2016. Dopamine Reward Prediction Error Coding. (Dialogues in Clinical Neuroscience)
Salvi et al., 2021. ADHD and Bipolar Disorder in Adulthood: Clinical and Treatment Implications. (Medicina)
Teicher et al., 2010. Hurtful Words: Association of Exposure to Peer Verbal Abuse With Elevated Psychiatric Symptom Scores and Corpus Callosum Abnormalities. (American Journal of Psychiatry)
Lang, 2000. The Limited Capacity Model of Motivated Mediated Message Processing. (Journal of Communication)
Meshi et al., 2013. Nucleus Accumbens Response to Gains in Reputation for the Self Relative to Gains for Others Predicts Social Media Use. (Frontiers in Human Neuroscience)




Comments